In recognition of World Hearing Day, March 3, the Academy’s Health-Care Relations Committee wants to share some helpful information and tips to manage wearing a mask and communicating with patients.
By Katharine A. Williams, Rebecca Henning, Jessica Spratt Novak, Margaret Kettler, Brittany Kyzer, and Emily Venskytis
The masking dilemma. We know it is imperative that we wear masks to protect our health and stop the spread of COVID-19, but no one is addressing what wearing a mask is doing to our ability to communicate, especially when the person has a hearing loss.
When we talk about hearing, there is low-pitch hearing that indicate our vowel sounds in speech. These low-pitch speech sounds produce the power of speech or volume in speech. High-pitch speech sounds are our important consonant sounds; these consonants are soft and give us the clarity of speech (the difference between mouSe and mouTH) and improve our ability to figure out what word someone is speaking.
When we put a mask over our mouths, regardless of what kind, it prevents those soft consonant sounds from escaping through or around the mask, automatically making it more difficult to understand what someone is saying. Even with normal hearing, speech coming from a person wearing a mask can sound like the adults from the Peanut cartoons; “I can hear you speaking, but I have no idea what you are saying!”
Not only do masks muffle speech and take away clarity by preventing the consonant sounds from being heard, masks also take away our ability to use visual clues that we have come to rely on. Whether you think you read lips or not, a lot of speech information comes from a person’s facial expressions and the placement of the mouth when saying a word.
Mouth movements and facial expressions are particularly useful when the speaker is talking quietly or in the presence of background noise. In these challenging listening situations, the placement of the speakers’ mouth can help the brain distinguish consonant-vowel combinations such as “ba,” “ga,” and “da.”
It is normal to feel some frustration understanding what someone is saying while wearing a mask, but if you feel you are having more trouble than others, it might be time to see an audiologist. In a world with masks, a mild hearing loss becomes a moderate hearing loss. Your brain must fill in more blanks your ears can no longer provide, decreasing your energy level and reducing your short-term memory. When you must focus on what someone is saying, your brain spends its energy decoding instead of remembering. A simple amplifier or hearing aids can help with these issues.
If you already wear hearing aids and are having more difficulties understanding, schedule an appointment to see your audiologist; there are special programs that can be added to help you regain some of the missing clarity the mask is taking away. There are also remote microphones and accessories that can be added to your hearing aids that will amplify a person speaking, and add the much needed clarity to speech.
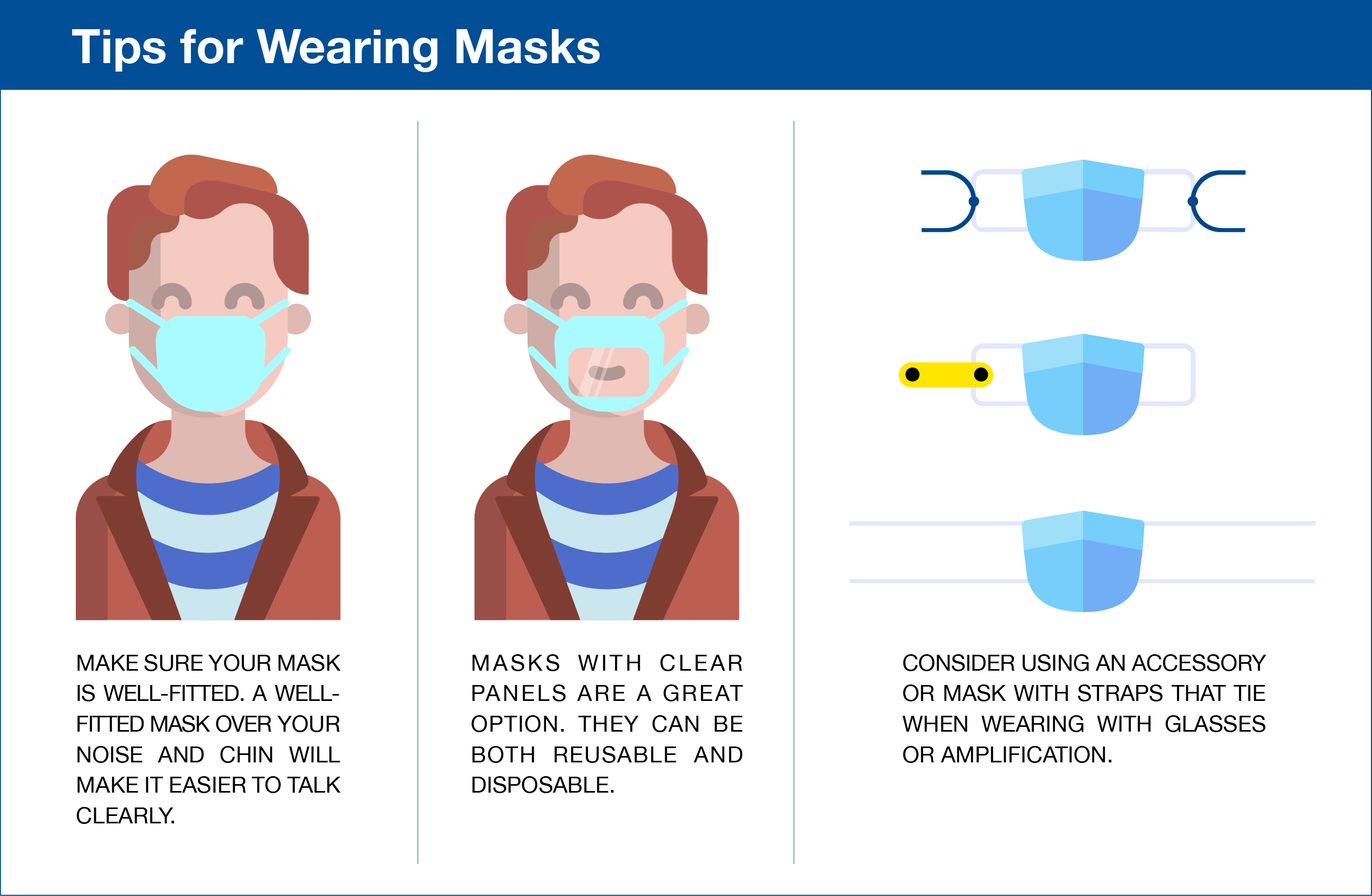
And if possible, ask or provide your loved ones with the surgical type masks; research has shown these provide the least amount of speech attenuation, so less clarity is lost. Or ask the person speaking if they have a clear mask; these masks attenuate speech the most but provide the speech clues on the face we often need to understand the difference between words.
If you are speaking to a person with hearing loss, raise your voice, but do not yell. Take pauses between words so the person’s brain can use context clues to fill in the blanks and catch up. Never speak while walking away. Wear surgical masks or clear masks. And advocate they seek help from an audiologist for reprogramming or accessories.
For a hearing aid user, wearing a mask can cause additional issues and fear the hearing aid might fall off. We have provided an additional page that shows tips for getting the mask off your ears and away from the hearing aids. We also provide ways to remove the mask off the ear without disturbing the hearing aid. And if all else fails, advocate for yourself. “I have a hearing loss, could you please speak louder?” Make sure to let the person know they should face you when speaking so speech is coming directly towards you and not decreased by having to travel around the person or from another room. And if you hear part of the sentence, ask the person to fill in the blanks: “I heard we are having dinner at six? Is that correct?”
You may have also seen or heard the joke of people complaining they themselves cannot hear when wearing a mask. This is because the mask not only muffles speech from others, it also muffles your own speech making a person feel they cannot hear themselves. For a person with hearing loss, not being able to hear themselves speak can be frustrating and stressful. Please be kind and patient and remind a person that you can hear them even if they cannot hear themselves.
Hearing loss by itself can be isolating, adding a mask can make this worse. If you have other tips or tricks that you have found helpful for you or a loved one, please let us know. We are all in this together!
All authors are members of the Academy’s Health-Care Relations Committee. Dr. Kyzer is the committee’s chair.
Katharine Williams, AuD, is an adult amplification audiologist at Vanderbilt University Medical Center.
Rebecca Henning, PhD, is a professor of audiology at University of Wisconsin-Stevens Point.
Jessica Spratt Novak, AuD, is a pediatric audiologist at Children’s Minnesota.
Margaret Kettler, AuD, is a clinical Manager/Division of Audiology, at Cincinnati Children’s Hospital Medical Center.
Brittany Kyzer, AuD, is a clinical audiologist at University of Louisville Health.
Emily Jo Venskytis, AuD, is an audiologist at UPMC Children’s Hospital of Pittsburgh.
Recent Posts
Medicaid Work Requirements Rule Could Affect Access to Hearing Healthcare
The Centers for Medicare and Medicaid Services (CMS) recently issued an Interim Final Rule implementing Medicaid work requirements for certain adult beneficiaries beginning in 2027….
Sleep in U.S. Adults
Previously, we reported on sleep routines and tiredness in children. You may now be wondering how well adults sleep. If so, a recent report by…
Audiology CPT® Codes Enter Routine AMA RUC Review Process
Over the next several months, a significant number of CPT® codes used to report audiology function tests will undergo review through the AMA/Specialty Society Relative…