By Samuel R. Atcherson, Evan T. Finley, B. Renee McDowell, and Celeste Watson
This article is a part of the November/December 2020, Volume 32, Number 6, Audiology Today issue.
Because of COVID-19 and broad mandates to wear face coverings, there are numerous local, state, and national conversations regarding communication access for individuals who are deaf and hard-of-hearing (DHH) in school, hospital, and public settings. Although there was an initial shortage and concerns about meeting global demands, we have witnessed, in a short period, rapid production of various types of masks and shields intended for use by either the public or health workers, including masks with clear (transparent) windows.
The major problem is that typical masks (cloth or medical) present an obvious visual barrier to those who depend on nonverbal communication cues on the face (e.g., mouth, lips, teeth, tongue, and cheeks) (Mendel et al 2008; Atcherson et al, 2017; Atcherson and Finley, 2019; Eby et al, 2020; Baltimore and Atcherson, 2020).
Indeed, both linguistic and nonverbal information are important for understanding social communication and interaction (Rieffe and Terwogt, 2000; Most and Aviner, 2009). In a timely publication concerning medical masks, Goldin et al (2020) reported acoustic degradations where medical masks act as lowpass filters and high frequencies between 2000-7000 Hz are attenuated by about 3-4 dB for simple surgical masks and up to 9-12 dB for N95 masks.
They cautioned that these reductions would prove challenging for DHH individuals when listening to speech in background noise and in reverberant (echo-like) settings—especially with advancing age and greater likelihood of hearing loss.
Mendel et al. (2008) recorded passages by a male speaker wearing a mask and presented those with and without pre-recorded dental office noise to listeners with normal hearing and moderate hearing loss in an audio only format. When the passages were presented in quiet, the simple surgical mask did not influence speech understanding. Not surprising, however, the dental office noise did have a detrimental effect on speech understanding. These authors considered the possibility that listeners with greater degrees of hearing loss might have more difficulty with masks as the reliance on visual cues increased.
Atcherson and colleagues (2017; 2019) conducted the first comparison of the standard surgical mask with a prototype transparent mask (prototype FaceView mask) and found that the transparent mask improved speech understanding in noise by making the lips and mouth visually accessible. In their studies, listeners in both the moderate and severe-to-profound hearing loss groups benefited, with the greatest magnitude of benefit observed for the severe-to-profound group. None of these studies, however, have considered the impact of transparent masks and their use with or without face shields.
In terms of the availability of transparent medical masks, the demand has far exceeded the supply. There are likely to be further supply challenges for these items as many schools and universities anticipate reopening. One commercially available transparent medical mask that has been around for nearly two years is The Communicator by Safe ‘N’ Clear, which is a Food and Drug Administration (FDA) Registered ASTM Level 1 surgical mask.
Safe ‘N’ Clear has experienced a surge in orders, and they continue to carry a backlog fulfilling orders as quickly as they can. They hope to meet the demand as quickly as they can. The only caveat about The Communicator is that it is not an N95-style mask that would be safe enough to use with COVID-19 patients. Not too long after COVID-19 arrived, two other transparent options became available. They include the Humanity Shield by Rapid Response PPE (i.e., personal protection equipment) and The Clear Mask, but only the latter is FDA-cleared as a class II surgical clear mask that meets ASTM Level 3 standards.
The Humanity Shield includes a full-face shield with draping fabric to cover the sides of the face and below the chin and can be used with a mask underneath. The Clear Mask is a face shield that covers the nose and mouth, but not the eyes. The manufacturers of these two newer offerings are also taking orders as well and may be delayed in production as demand surges. Therefore, those awaiting viable transparent mask options are looking for acceptable alternatives and safe PPE combinations, such as cloth coverings (with and without transparent options) and face shields. TABLE 1 lists some of the transparent masks and face shields relevant to this topic. The reader will note that there are a variety of transparent cloth masks sold by various vendors, including patterns to try to make your own.
| MANUFACTURER | DESCRIPTION |
| Safe ‘N Clear | Transparent Surgical-Style Mask (FDA Registered), available but backordered |
| Rapid Response PPE | Face Shield with Drop Cloth |
| ClearMask | Face Shield for Mouth and Nose |
| FaceView | Transparent Respirator-Style Mask, not commercially available |
| LEAF Mask | Transparent Mask (FDA Registered), not commercially available |
| HelloMask | Transparent Surgical-Style Mask, not commercially available |
| Various Cloth Masks | Commercial and Do-It-Yourself Transparent Cloth Masks by Catharine McNally and Dr. Tina Childress |
| Accessible Masks | Accessible masks with transparent face coverings by Jacob deHahn and Patrick deHahn. |
Preliminary Data on Masks and Masks Plus Shields
The avalanche of interest in transparent face coverings has us wondering about the possible effect of transparent masks and/or face shields on speech acoustics. Recently, we collected preliminary data on some masks available to us (e.g., standard surgical mask, KN95 mask, N95 mask (vented), prototype FaceView transparent mask, Safe ‘N’ Clear’s transparent surgical mask, and handmade transparent cloth mask). We presented white noise through a fabricated loudspeaker manikin head, and we recorded the output from 6 feet in a double-walled sound booth.
| DEVICE | MASK ONLY | MASK + SHIELD |
| Surgical Mask | 5.0 dB | 20.0 dB |
| KN95 Mask | 8.7 dB | 29.2 dB |
| N95 Mask | 10.9 dB | 28.7 dB |
| FaceView Mask (transparent window) | 12.0 dB | 24.9 dB |
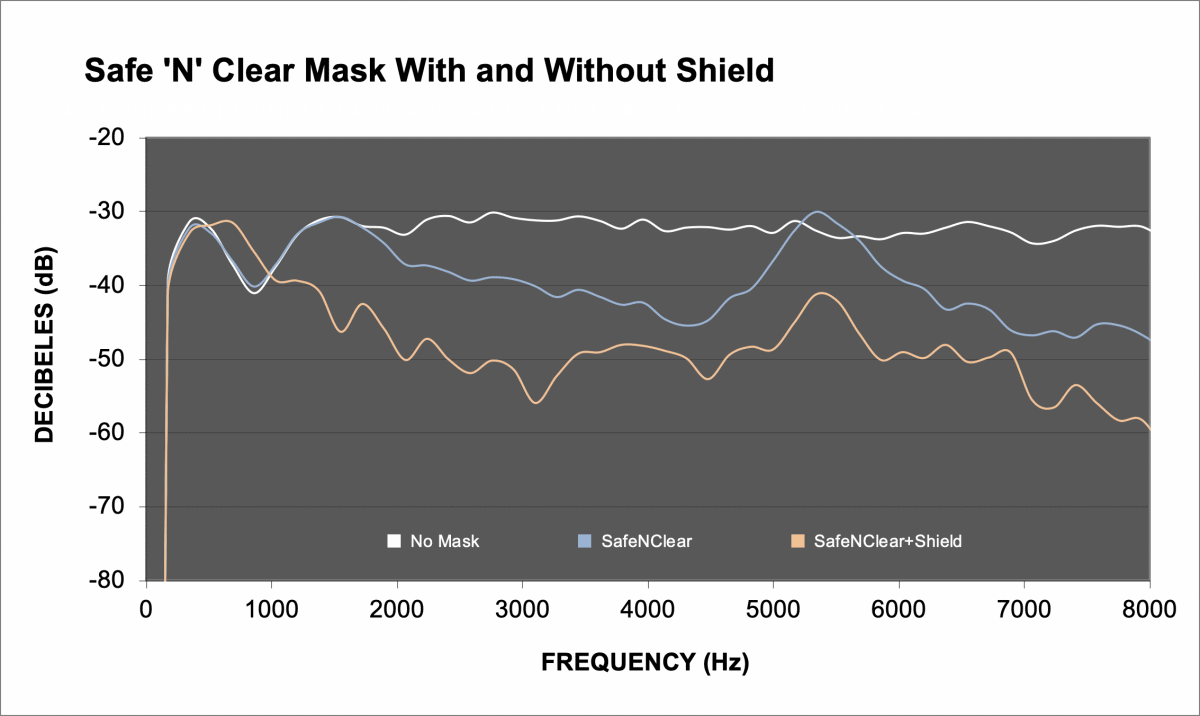
| Safe ‘N’ Clear Mask (transparent window) | 13.3 dB | 24.7 dB |
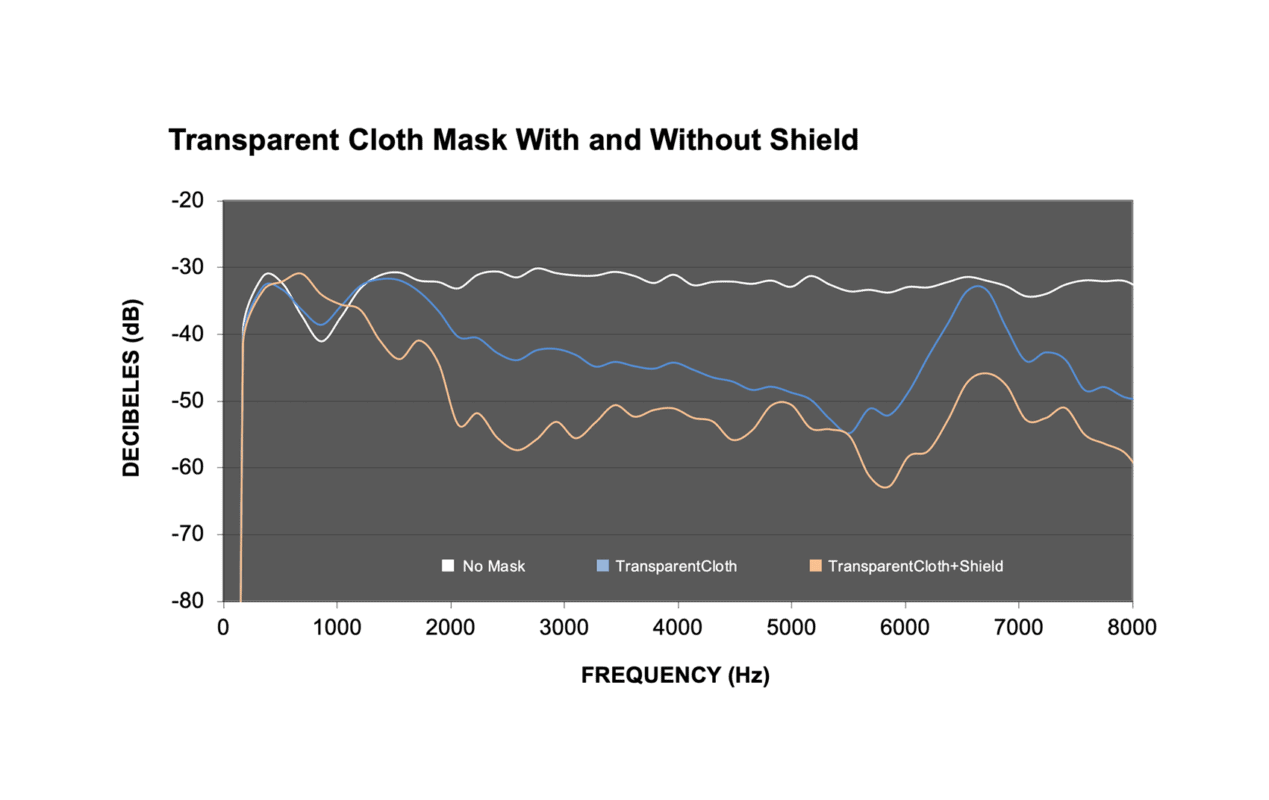
| Transparent Cloth Mask | 21.2 dB | 29.2 dB |
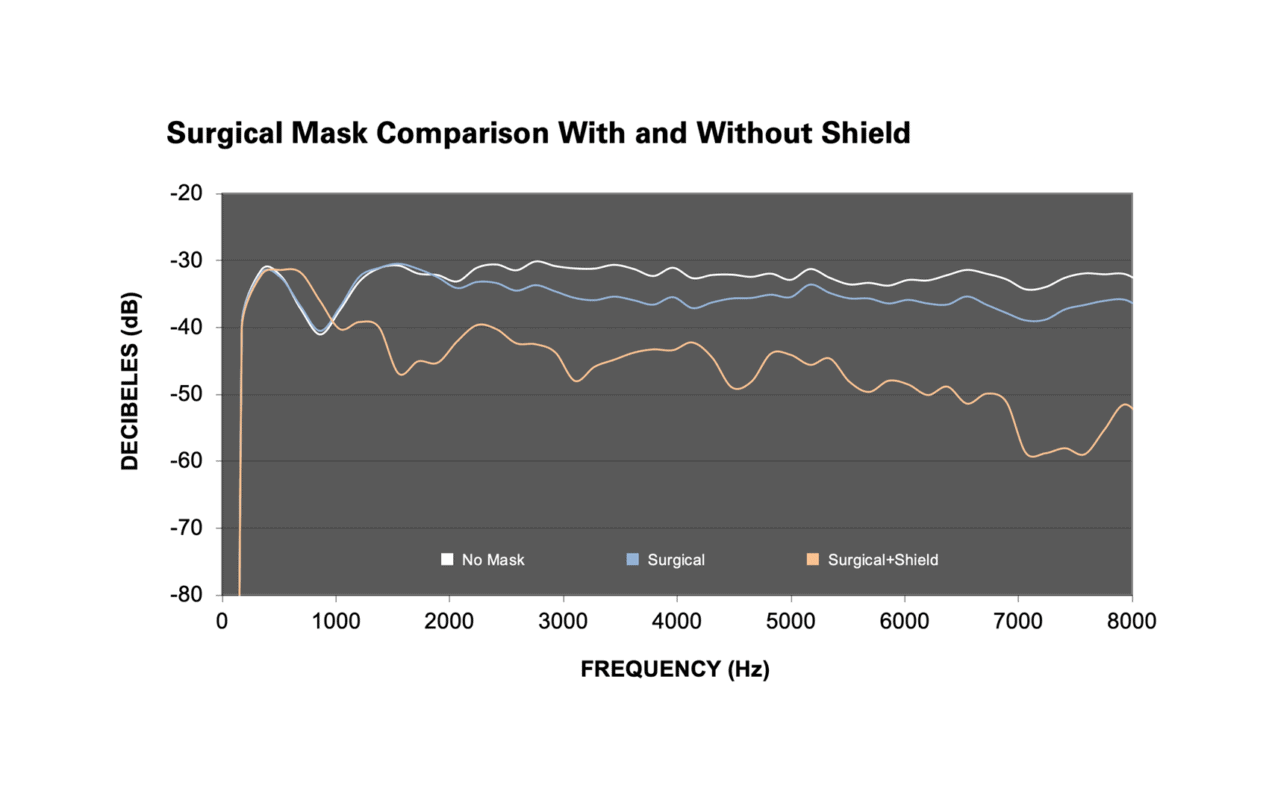
FIGURE 1. Standard surgical mask with (orange line) and without (blue line) a face shield. White line is the reference ‘no-mask’ condition. From upper to lower y-axis, decibels (dB) are arbitrarily reported from high intensity (-20 dB) to low intensity (-80 dB).
This resonant peak is believed to coincide with vibrational distortions produced by the film. As examples, FIGURES 1 THROUGH 3 illustrates visually how some of the masks with and without a face shield perform. In these figures, the y-axis is reported arbitrarily in SPL from high intensity (-20 dB) to low intensity (-80 dB). The white line, representing the no-mask condition, has the highest SPLs. The blue line, representing the masks only condition, has the next highest SPLs. Finally, the orange line, representing, the mask plus shield condition, has the lowest SPLs. These levels can now be compared to the data reported by Goldin et al (2020).
Conclusion
Although transparent masks were shown to reduce SPL and conceivably further degrade speech more than their non-transparent counterparts, they play an important role in preserving nonverbal communication cues on the face.
Without a doubt, transparent masks used with or without shields help maintain access to the mouth, which can help to aid some listeners with lipreading and other nonverbal cues, such as emotion (McIntosh and Howell, 2020; Atcherson, 2020; Most and Aviner, 2009). However, some individuals depend more heavily on the quality of speech whether or not there is a transparent window.
Additionally, new knowledge about further sound pressure reductions by transparent masks, with or without shields, raises several considerations:
- Do we use more vocal effort with different types of mask materials?
- Are we exaggerating our speech through certain types of mask materials?
- Does speaking with a mask cause our masks to shift, requiring repeated adjustments?
- Subsequently, do we enunciate less to reduce mask shifting?
- Do we speak less loudly when we wear shields (sound reflection back towards our ears)?
- What is the effect on listening with increased distance between two people talking while wearing masks and/or face shields?
- Are all people good at reading nonverbal cues?
- Does communication with non-transparent masks increase cognitive effort and fatigue?
- Do hearing aids and implantable devices compensate or adjust to mask-related decibel changes?
- Is there any value in considering supplemental acoustic access, such as using hearing assistive technology systems (HATS), including remote microphone technologies?
- Are there groups other than those who are DHH who could benefit from transparent masks?
- Will children with normal hearing benefit from teachers wearing transparent masks?
- Will it help to have interpreters wear transparent masks (e.g., foreign languages and American Sign Language)?
All these questions are important to think about when considering communication in a holistic manner. In other words, what do we lose with non-transparent masks vs. what do we gain with transparent masks and face shields? These questions remain to be answered, and we are forced to consider them in the middle of a COVID-19 pandemic that may be here to stay a while into the foreseeable future.
References
Atcherson SR. (2020, Winter) I can hear AND see what you’re saying. Hearing Health Magazine 36(1):24-25.
Atcherson SR, Finley ET. (2019, June 1-4) Research on Stethoscopes and Facemasks: Implications for Hearing Loss and Healthcare. Presentation at the 2019 Association of Medical Professionals with Hearing Losses/American Deafness and Rehabilitation Association conference, Baltimore, MD.
Atcherson SR, Mendel LL, Baltimore WJ, Patro C, Lee S, Pousson M, Spann MJ. (2017) The effect of conventional and transparent surgical masks on speech understanding in individuals with and without hearing loss. J Amer Acad Audiol 28(1):58-67.
Baltimore WJ, Atcherson SR. (2020, June 1) Helping our clients parse speech through the mask during COVID-19. The ASHA LeaderLive. Accessed on July 7, 2020 https://leader.pubs.asha.org/do/10.1044/leader.MIW.25062020.34/full/
Eby TL, Arteaga AA, Spankovich C. (2020) Otologic and audiologic considerations for COVID-19. Otolaryngol Head Neck Surg 163(1):110-111.
Goldin A, Weinstein B, Shiman N. (2020) How Do Medical Masks Degrade Speech Reception? Hear Rev. Accessed on April 5, 2020, https://www.hearingreview.com/hearing-loss/health-wellness/how-do-medical-masks-degrade-speech-reception
McIntosh, A. & Howell, R. (2020, June 19). ADA and facemask: are you ADA-effective? LinkedIn. Accessed on July 23, 2020, https://www.linkedin.com/pulse/ada-compliance-facemask-you-compliant-dr-anne-mcintosh?trk=related_artice_ADA%20and%20Facemask%3A%20Are%20you%20ADA-Effective%3F%20_article-card_title
Mendel LL, Gardino JA, Atcherson SR. (2008) Speech understanding using surgical masks: a problem in health care? J Amer Acad Audiol 19(9):686-695.
Most T, Aviner C. (2009) Auditory, visual, and auditory–visual perception of emotions by individuals with cochlear implants, hearing aids, and normal hearing. J Deaf Studies Deaf Ed 14(4):449-464.
Rieffe C, Terwogt MM. (2000) Deaf children’s understanding of emotions: desires take precedence. J Child Psychol Psych 41:601–618.